Services on Demand
Article
Bookmark
TropIKA.net
On-line version ISSN 2078-8606
TropIKA.net vol.1 no.1 Jan./Mar. 2010
A review of clinical trials of treatments for visceral leishmaniasis in the Indian subcontinent (India, Bangladesh and Nepal)
Messiah M CheeranI; Shyam SundarII; Sumar RijalIII; Abul FaizIV; Pascal MilletI; Piero L OlliaroV
IUniversité Victor Segalen Bordeaux 2, France
IIInstitute of Medical Sciences, Banaras Hindu University, Varanasi - 221005, India
IIIB P Koirala Institute of Health Sciences, Dharan, Nepal
IVDirector General of Health Services, Bangladesh
VUNICEF/UNDP/WB/WHO Special Programme for Research and Training in Tropical Diseases (TDR), Geneva, Switzerland
Date of database searches: May 2008.
ABSTRACT
BACKGROUND: India, Bangladesh and Nepal share nearly 60% of the global burden of the 500,000 annual cases of visceral leishmaniasis (VL, kala-azar). In 2005, the three countries and the World Health Organization (WHO) signed an agreement to eliminate VL as a public health problem from this region by 2015.
OBJECTIVES: To conduct a review of clinical trials of the treatment of VL in India, Bangladesh and Nepal, in order to contribute to the evidence base for the treatment options to be used in the VL elimination programme.
METHODS: We searched PubMed and trial registry databases and contacted clinical investigators to identify published and unpublished comparative, non-comparative and dose-finding trials of amphotericin deoxycholate or liposomal (AmBisome®), miltefosine, paromomycin, sodium stibogluconate and paromomycin + sodium stibogluconate for the treatment of VL in the three countries. Efficacy evaluation was based on final cure at six months of follow up or longer. We reviewed reported serious adverse effects or adverse effects and laboratory changes. The methodological quality of studies was assessed. Six-month success rates were recalculated with 95% confidence intervals (95%CI) on both an intention-to-treat (ITT) and a per-protocol (PP) basis. Relative risks (RR, fixed effect) with 95%CI for failure were calculated for comparative studies.
MAIN RESULTS: Twenty-three (23) clinical trials enrolling 5,730 patients met the inclusion criteria: 11 comparative, four non-comparative, eight dose-finding. Both plain and liposomal amphotericin B (AmBisome®) were effective in these trials. Miltefosine is as effective as amphotericin B and is the only drug that has been tested in a Phase 4 study; in these conditions, effectiveness was lower than efficacy. Paromomycin is effective both alone and combined with sodium stibogluconate, and was shown not to be different from amphotericin B using a non-inferiority trial design. Sodium stibogluconate is lost to parasite resistance in Bihar; recent data from other areas were not available. The major adverse events were cardiotoxicity with sodium stibogluconate; ototoxicity and nephrotoxicity for paromomycin; vomiting and diarrhoea for miltefosine; nephrotoxicity, vomiting and diarrhoea for amphotericin B deoxycholate and infusion-related fever and chills with AmBisome.
CONCLUSIONS: AmBisome, miltefosine and paromomycin are effective options for treatment of VL in the Indian subcontinent. Other factors, such as costs, and practicalities of care and delivery need to be considered for policy decisions. The majority of available evidence was from Bihar, India with very limited evidence from Bangladesh and Nepal, except on sodium stibogluconate. More studies are needed in these countries to test the efficacy, safety and effectiveness of the various treatment options.
Introduction
Visceral leishmaniasis (VL, kala-azar or "black fever") is a fatal systemic disease if untreated. VL is caused by various species of the protozoan parasite Leishmania and is responsible for approximately 59,000 deaths per annum and approximately 2.4 million disability adjusted life years (DALYs) lost (1,2,3). Of the annual incidence of 500,000 cases, approximately 300,000 (60%) occur in India, Bangladesh and Nepal. (2,3). The actual incidence of VL in the Indian subcontinent is considered to be at least eight to ten times higher than the reported case numbers (2,5). Approximately 150 million people living in some 94 districts of the India, Bangladesh and Nepal at risk of contracting VL (3). See also Figures 1-3.
In the Indian subcontinent, VL is anthroponotic (i.e. carried by humans and transferred to other animals). While this feature, along with the recent development of new diagnostics and therapeutics, creates an opportunity to control and eliminate the disease, it is also conducive to the spread of resistance as, when resistant strains occur in these conditions, they can be re-circulated rapidly (3).
The theoretical basis for VL elimination in the Indian subcontinent is: (i) human beings are the only reservoir; (ii) there is only one vector species, which can be controlled; and (iii) the geographical distribution is limited and quite well defined. The ministers of health of Bangladesh, India and Nepal signed a memorandum of understanding (MOU) in Geneva in 2005 for joint efforts to eliminate VL from the Indian subcontinent by the year 2015 (3,7). The target is to reduce the annual incidence of VL in the endemic regions to less than one per 10,000 population, at the district level or sub-district level by 2015 (7).
Successful elimination of VL, will reduce poverty and promote equity, and advance the socio-economic development of the region (3). VL elimination also has relevance to the Millennium Development Goals: prioritized intensification of control of neglected tropical diseases will contribute directly to the reduction of the communicable disease burden (Goal 6, Target 8) and indirectly to efforts to reduce poverty and hunger (Goal 1). Current treatment modalities include amphotericin B, AmBisome and other lipid formulations, miltefosine, paromomycin, and sodium stibogluconate. Parasites have become resistant to antimonials in Bihar, India and possibly neighbouring parts of Nepal, but there appears to still be sensitivity in other parts of Bangladesh, India and Nepal. (5,9-11).
Objectives
To document, analyse and review the safety and efficacy profiles of drugs used for the treatment and control of VL in the Indian subcontinent, namely, amphotericin B deoxycholate, liposomal amphotericin B (AmBisome), miltefosine, paromomycin, sodium stibogluconate and paromomycin + sodium stibogluconate.
A previous systematic review of clinical trials of treatments of VL in India (4) covered research conducted during the period 1980-2004. The present review aims to update the previous review by including information on the clinical trials conducted in Bangladesh and Nepal, in order to produce reliable summaries of safe and effective regimens to support policy or research decisions specifically in the context of the elimination programme.
Methods
Inclusion and exclusion criteria
Criteria for inclusion in this review were established in advance as: trials of any design; involving the use of any of the named drugs (amphotericin B, AmBisome, paromomycin, miltefosine, sodium stibogluconate and paromomycin + sodium stibogluconate); for the treatment of leishmaniasis in any patient group; conducted in India, Bangladesh and Nepal in the period 1990 to 2008; and reporting six-month cure rate as an outcome.
Trials for other VL drugs – such as pentamidine, sitamaquine, amphotericin B colloidal dispersion (ABCD), amphotericin B Lipid Complex (ABLC), and liposomal amphotericin B other than AmBisome – were excluded from this review, as these are now considered to be obsolete and have no relevance to the elimination programme.
Pentamidine has been abandoned in India due to declining efficacy and unacceptable toxicity (irreversible insulin dependent diabetes and death). More studies are needed to evaluate sitamaquine, as it seems to have clinical efficacy that warrants further development. AmBisome is the best tolerated among all lipid formulations of Amphotericin B (50).
Non-comparative trials are uncontrolled trials where all patients receive treatment with the same drug, with no control group. Such trials are not included in most systematic reviews but we decided that it was important in this review to consider all data available on drugs relevant to the VL elimination programme.
Our criteria for 'cure' were clinical cure (when fever subsides, general condition of the patient improves and spleen regresses) and/or parasitological cure (absence of parasites in spleen or bone marrow aspirate).
Data on adverse effects were also included where available.
Search strategies
We searched PubMed and the clinical trial registries of WHO and the US National Institutes of Health (www.clinicaltrials.gov) using the keywords: "clinical trials", "visceral leishmaniasis", "kala azar", "India", "Bangladesh", "Nepal". In addition the targeted study drugs were included: "AmBisome", "amphotericin B deoxycholate", "miltefosine", "paromomycin", "and sodium stibogluconate". The last online search was done on 21st May 2008. We also contacted investigators, who were asked if they were aware of trials which might have been missed or were yet to be published.
No language restrictions were imposed in the search but it should be noted that English is the official language for research and clinical trials in the Indian subcontinent.
Quality assessment
We assessed for quality all studies identified as meeting the inclusion criteria. For controlled trials, the methods used for randomization were considered. Other aspects of the trials which we considered might affect the reliability of the results were also noted These included non-specification of randomization methods (13,15,19 & 27), high proportion of trial participants lost to follow-up (27), and non-specification of allocation (17,20).
Data extraction and synthesis
Extracted data were cross checked for accuracy and entered into Excel spreadsheets. Six-month success rates were (cure rates at six-month follow up) calculated with 95% confidence intervals out of the enrolled patients (intent-to-treat, ITT) and the evaluable patients (per protocol, PP) populations. The calculations were based on ITT analysis. Therefore the denominator was the total patients enrolled, irrespective of whether they were followed up or evaluated. PP only included the number of evaluable patients in the denominator. Results were presented in both tabular and graphical form.
For comparative studies, data were entered in RevMan (Cochrane Information Management System, http://www.cc-ims.net/RevMan) and relative risks (fixed effect) with 95%CI for failure were calculated. Heterogeneity (chi2-, I2) and overall effect (Z test) were measured.
Results
We identified a total of 105 publications of which 104 were published online. One study was identified on the advice of the investigators whom we contacted.
We excluded 82 publications: 27 which were not clinical trials; 18 which were clinical trials of drugs not included (sitamaquine, pentamidine, amphotericin B lipid complex, amphotericin B colloidal dispersion, atovaquone, ketoconazole, fluconazole, roxithromycin, verapamil, INH, rifampicin, ethambutol, etc.); seven clinical trials which were either ongoing or recently completed and not published; and another 30 publications for other reasons (diagnostic and interventional trials). All the included studies were in English; all the VL studies found in other languages concerned other parts of the world.
We extracted data from the remaining 23 clinical trials. Of these, 11 were comparative, four non-comparative, and eight were dose-finding studies, The selection process is shown as a flowchart in Figure 4.
Quality assessment of included studies
Methods of allocation were not applicable to the four non-comparative trials included in this review (23-26), as these were uncontrolled studies where all patients received the same treatment.
In one dose-finding study (Chowdhury SB 1993),(27), the method of randomization was not specified. This study was open-labelled and there was no concealment of treatment allocation. Two other dose-finding studies (28,33) patient allocation was done in sequential groups. One dose-finding study by Karki et al. (29) was open-label with no concealment of allocation. Two studies (Sundar AmphB, 15d vs alt day 2007 and Thakur AmBi, 3 regimens 1996) (32,34) were open-label, having computer generated randomization and no concealment of treatment. One study (Sundar AmBi single vs daily 2001) (30) was open-label, had computer generated randomization with treatment concealment. Another study (Sundar AmBi, 3 regimens 2002) (31) was double blinded, with computer generated randomization and treatment concealment.
For three randomized, open-label comparative studies (Mishra AmphB vs SB 1994, Sundar AmphB vs Par2007, and Thakur AmphB vs SB 1993), (13,15,19) the method of randomization was not specified. For two randomized open-label studies (Thakur AmBi vs AmphB 2001) and Thakur AmphB vs SB 2004 (17,20) the allocation was not specified, but the authors reported having matched patients by age and sex. Two randomized open-label studies (Jha PM vs SB 1998 and Thakur PM+SB vs SB 2000) (12,22) had computer generated non-concealed allocation. Another two randomized open-label studies (Sundar AmphB, Conv vs lipid 2004 and Thakur PM vs SB 2000) (16, 22) had computer generated concealed allocation. One open-label comparative study (Sundar AmphB vs Milt 2002) (18) with non-concealed allocation was randomized using blocks in the ratio 3:1. Another open-label comparative study (Singh AmphB vs Milt 2006) (14) having non-concealed allocation was randomized using slips. After quality assessment it was found that some studies provided more reliable evidence than the others, but none of the studies were excluded on quality grounds.
Included studies
Tables 1 and 2 detail studies included and their characteristics respectively.
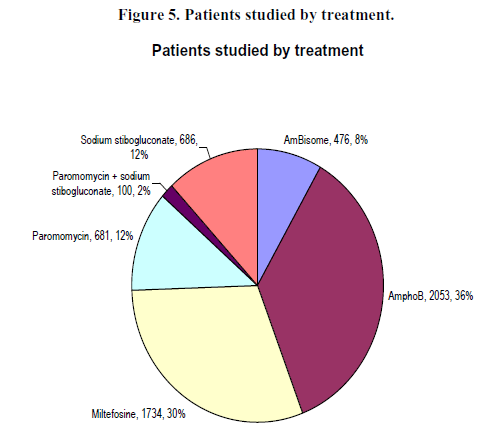
Table 3 summarises information on the patients enrolled in the included studies, overall and by treatment. Table 4 shows patients enrolled, in total and by treatment, contributing to the intent-to-treat and per-protocol datasets. Breakdowns of patients studied are also shown in Figures 5 and 6.
Crude efficacy and safety outcomes
Efficacy outcomes (six-month success rates in comparative and non-comparative trials) are shown in Table 5 and 6, and safety outcomes in Table 7.
Comparisons are presented using Forest plots (Figure 7) and L'Abbé plots for success rates with bubble proportional to the sample size (enrolled patients) (Figure 8).
Sodium stibogluconate
We identified nine clinical trials (13 study arms) of which two were dose-finding, six comparative and one non-comparative. Sodium stibogluconate is the only drug for which trials have been done in Bangladesh and Nepal. We identified two studies from Nepal (one non-comparative and one dose-finding study) (25,29) and one from Bangladesh (dose-finding study with four arms, Chowdhury SB 1993 (27). A total of 686 (12% of database) patients received sodium stibogluconate. 558 patients (10.4% of database) were evaluable and hence 81.3% of patients on sodium stibogluconate were evaluable based on ITT. Of these, 285 (5%) were in comparative trials, 281 (4.9%) in dose-finding trials and 120 (2.1%) were in non-comparative trials.
SB 1993, (27) the only study from Bangladesh had four arms; the randomization method was unspecified; the six-month cure rates were 28.8% and 68% (sample size 59, 10 mg/kg/day for 20 days single twice daily); 39.6 and 72.4% (53 patients, 20 mg/kg/day for 20 days single daily dose); 36.4% and 83.3% (55 patients, 10 mg/kg/day for 10 days single twice daily); 38.3% and 85.2% ( 60 patients, 20 mg/kg/day for 10 days single daily dose) by ITT and PP respectively.
Karki SB 1998 (29) (dose-finding, two arms) and Rijal SB 2003 (non-comparative) (25) were the studies from Nepal. For Karki SB 1998 (29) the cure rates were 77.8% and 77.8% (27 patients, 20 mg/kg/day for 20 days); 92.6% and 92.6% (27 patients) by ITT and PP respectively. For Rijal SB 2003 (25) the cure rates were 82.5% and 85.3% (120 patients, 20 mg/kg/day for 30 days) by ITT and PP respectively.
Five comparative trials were from India. Cure rates were: Mishra AmphB vs SB 1994 (13) = 62.5% and 62.5 % (40 patients) by ITT and PP respectively; Thakur AmphB vs. SB 1993, (19) = 76.0% (75 patients) by both ITT and PP; Thakur AmphB vs. SB 2004 (20) = 46.7% (60 patients) by both ITT and PP; Jha PM vs. SB 1998, (12)= 63.3% and 63.3% (30 patients) by ITT and PP respectively; Thakur PM vs. SB 2000 (21) = 66.7% and 69% (30 patients) by ITT and PP respectively; Thakur PM+SB vs. SB 2000 (22) = 52% and 53.1% by ITT and PP respectively. (Table 3 and Figure 9.)
Safety: Myocarditis and cardiotoxicity were reported in five trials. Thakur AmphB vs SB 2004 had nine cases of cardiotoxicity (15%), two of these were fatal (3.3%). Rijal SB 2003 reported four cases of cardiotoxicity (3.3%), two of these fatal (1.7%) and the other two required shifting to amphotericin B. Myocarditis not needing treatment discontinuation was reported in two patients each by Jha PM vs SB 1998 and Thakur PM vs SB 2000 (6.7% in both studies) and one (2%) by Thakur PM+SB vs SB 2000. Overall, 18 patients (2.6%) had myocarditis or cardiotoxicity of 686 patients who had sodium stibogluconate, and four died (0.6%, with a fatality rate of 22%)
Other adverse events were bleeding (24 cases, 3.4%, including two deaths from severe bleeding, all from Chowdhury SB 1993), splenic infraction (one death, 0.15%, from Chowdhury SB 1993), one death (0.15%) due to unexplained shock, one sudden death (0.15%) on the last day on injection, arthralgia (15 cases from two studies, 2.2%), anorexia (32 cases from four studies, 4.7%), icterus (two cases, 0.3%), rash (eight cases, 1.2%), vomiting (one case, 0.15%), elevation of AST (5 cases, 0.75%), ALT (four cases, 0.6%) and creatinine (one case, 0.15%), rigors (23 cases from two studies, 3.35%), suffocation (four cases, 0.6%), cellulites, thrombophlebitis, fever (22 cases, 3.3%), metallic taste (eight cases, 1.2%), neuritic pain (three cases, 0.45%).
In summary, of the 686 patients enrolled in nine trials of sodium stibogluconate, three (407 patients) reported nine deaths (as described above). Hence the estimated total mortality ranges from 1.3 to 2.2%.
Paromomycin
We identified three trials with seven arms (all trials were comparative) enrolling a total of 681 patients (11.9% of database) in paromomycin arms, of whom 676 (12.6% of database) were evaluable. Thus 99.3% of patients on paromomycin were evaluable based on PP. The arms 12mg/kg for 21 days, 16mg/kg for 21 days and 20mg/kg for 21 days (all 3 of Jha PM vs SB 1998 (12)) had six months ITT cure rates of 76.7%, 80% and 83.3% respectively. In the case of the three arms of 12mg/kg for 21 days, 16mg/kg for 21 days and 20mg/kg for 21 days (of Thakur PM vs SB 2000 (21)) the six-month ITT cure rates were 90% 93.3% and 96.7% respectively. The six-month ITT cure rate for 11mg/kg for 21 days (Sundar AmphB vs Par2007 (15)) was 94.6%. (Table 3 and Figure 10.)
Safety: Adverse events included ototoxicity (11 cases from three studies, 1.6%), nephrotoxicity (four cases, 0.6%), elevated AST (40 cases, 5.9%) and ALT (14 cases, 2%), vomiting (five cases from three studies, 0.75%), pain at injection site (276 cases, 40%) and fever (13 cases, 1.9%). (See Table 5.)
Paromomycin + sodium stibogluconate
We identified one trial (comparative) where two arms were paromomycin-sodium stibogluconate combinations (Thakur PM+SB vs SB 2000-(22)). There were 100 patients enrolled (1.7% of the database). All of them were evaluable (100% by ITT) and it constituted 1.9% of the total 5380 evaluable patients. The arms PM12mg/kg + SB20 mg/kg daily for 21 days and PM18mg/kg + SB20 mg/kg daily for 21 days had 6 months ITT cure rates of 92.3% and 93.8% respectively. (PP Cure rates 92.3% and 93.8% respectively.) (Table 3 and Figure 7.)
Safety: One case of myocarditis was reported (1%). Ototoxicity could not be evaluated as only 19 of 100 patients had audiometric assessment. (See Table 5.)
Miltefosine
Six trials were identified for miltefosine with 11 treatment arms (two comparative, two dose-finding and two non-comparative trials) enrolling 1734 patients (30.3% of the data base), of whom 1560 were available for evaluation by PP (29% of the database). Miltefosine trials comprised the second largest drug group with respect to number of patients after amphotericin B (35.8%).Three of these were paediatric trials.
The two comparative trials were Singh AmphB vs Milt 2006 (14) (two arms) and Sundar AmphB vs Milt 2002(18) (1 arm) with 363 patients (6.3% of database) (the former is discussed under pediatric trials). The trial Sundar AmphB vs Milt 2002 (18) had a cure rate of 94.3% and 96.9% by ITT and PP respectively (sample size 299).
There were 159 patients enrolled in the two dose-finding studies (2.8% of the database.) Jha Milt 1999 (28) had a total of 120 patients, with 30 patients each in four arms. The cure rates of the first two arms were 93.3% by ITT and PP (50 mg/day for one week, then 100mg/day for 3 weeks (a total dose of 2450 mg) and 50 mg/ day for six weeks (a total dose of 2100 mg) ) and the last two arms had a cure rate of 96.7% by ITT and PP (100 mg/day for one week, then 150mg/day for three weeks (total 3850mg) and 100 mg/day for 4 weeks (tot 2800mg) ).
Non-comparative trials accounted for the majority of patients for miltefosine trials (1212 patients, 21.2% of the total database). Of these, 1132 patients were from the Phase 4 trial, Bhattacharya Phase 4 Milt 2007 (24). The cure rates for this study were 81.9% and 95.5% by ITT and PP respectively.
Paediatric trials: Three paediatric trials were identified though this review; one each in the comparative, non-comparative and dose-finding categories.
The cure rates (miltefosine arms) for the comparative trial Singh AmphB vs Milt 2006 (14) were 93.2% and 97.6% respectively by ITT and PP for the arm with a sample size of 44 patients (those who had not received prior anti-leishmanial drug dose 2.5 mg/kg/day for 28 days). For the second arm with 20 patients (these patients had earlier received 30 days course of sodium stibogluconate at 20 mg7kg7day; dose 2.5 mg/kg/day for 28 days). The cure rates were 95% and 100% by ITT and PP respectively. The amphotercin B arms had a cure rate of 91.3% and 100% by ITT and PP respectively (38 patients) for group 1 (AmB for previously treated with SAG-1 mg/kg, cumulative dose 15mg/kg). Group 2 (AmB for previously untreated with SAG-1 mg/kg, cumulative dose 15mg/kg) had cure rates of 92.1% and 100%, respectively (23 patients).
The adverse events with miltefosine 2.5mg/kg/day (Groups 1 & 2) were: vomiting 23 cases; diarrhoea 26, anorexia 7; elevated ALT 39, AST 31, BUN 8; rash 2 . For amphotericin B (1mg/kg/day (Groups 3 & 4))adverse events were: anorexia eight cases; elevated ALT 32, AST 34, BUN 43; rash 8.
The non-comparative trial Bhattacharya Milt 2004 (23) with 80 patients had cure rates of 93.8% and 94.9% by ITT and PP respectively. The adverse events were: vomiting 21 cases(26%) of which 2 were CTC Grade 3-4 2.6%); diarrhoea 20 cases (25%), of which three were CTC Grade 3 (1.3%), elevated AST 44 (55%), one CTC Grade 3 (1%). No AE required discontinuing therapy.
The dose-finding study Sundar Milt 2003 (33) had two arms of 18 and 21 patients. The first arm had a cure rate of 83.3% and 88.2% by ITT and PP respectively (2.5 mg/kg/day for 14 days); the second arm had a cure rate of 90.5% by ITT and PP (1.5 mg/kg/day for 28 days). The adverse events were for miltefosine at 2.5 mg/kg/day x 28 d were: vomiting 7seven cases (33.3%); diarrhrea, anorexia, nausea, elevated ALT one case each (4.8%); for miltefosine at 1.5 mg/kg/day x 28 d: vomiting seven cases (38.9%) and diarrhoea three (16.7%).
Figures 11 depicts the ITT cure rates and Figure 12, ITT cure rates vs the PP cure rates of miltefosine.
Safety: Adverse events reported with miltefosine were mainly vomiting (261 cases from five studies, 15%), diarrhoea (180 cases from five studies, including one death from acute diarrhoea, 10.4% and 0.06% respectively), one death from abdominal pain and swelling (0.06%), elevation of AST (253 cases from four studies,14.6%), ALT elevation (195 cases from 3 studies, 11.3%), elevated BUN (eight cases, 0.45%), high creatinine, pneumonia, renal failure, Steven Johnson syndrome, rigors (one case each, 0.06% each) (See Table 5.)
Amphotericin B deoxycholate
Amphotericin B trials contributed the largest share of patients (2053 patients, 35.8% of the database) (Figure 5, Tables 1 and 2.) Of these 25.9% (1485) were from a dose-finding study Sundar AmphB, 15d vs alt day 2007 (32) with four arms. We identified eight comparative trials with nine arms and 568 patients (9.9% of the total database). Of the 2053 patients on amphotericin B (35.8%), 2012 were evaluable (37.4% of the evaluable patients, the largest study). No non-comparative study was identified for amphotericin B.
The cure rates by ITT and PP for the dose-finding study (Sundar AmphB, 15d vs alt day 2007) (32) were 95.5% and 97.1% (group A 245 patients receiving a dose of 1 mg/kg,15 infusions on alternate days), 92.2% and 96.2% (group B, 244 patients, dose of 0.75 mg/kg, 15 infusions, alternate days), 96.6% and 98.4% (group C 500 patients, dose of 1 mg/kg,15 infusions, daily), 96% and 97.7% (group D, 496 patients, dose of 0.75 mg/kg,15 infusions, daily)
The study Sundar AmphB vs Milt 2002 (18) had 99 patients on amphotericin B (1mg/kg, 15 infusions, alternate days) and the cure rates were 97% and 100% by ITT and PP respectively. The amphotericin B arm of the study Sundar AmphB vs Par2007 (15) had 165 patients (1 mg/kg, alternate days for 30 days) and cure rates were 98.8% and 99.4% by ITT and PP respectively. Cure rates for Sundar AmphB, conv vs lipid 2004(16) were 96.1% by both ITT and PP (51 patients, 1 mg/kg on alternate days for 30 days). The trial Thakur AmBi vs AmphB 2001 (17) had cure rates of 100% by both ITT and PP (17 patients) (1 mg/kg daily for 20 days).
The cure rates for Mishra AmphB vs SB 1994 (13) were 100% by both ITT and PP (40 patients receiving 0•5 mg/kg infused in 5% dextrose, 14 doses, alternate days) Cure rates for Thakur AmphB vs SB 1993(19) were 100% by both ITT and PP (75 patients on 1 mg/kg, starting with 0.5mg/kg, alternate days to reach 20mg/kg). The trial Thakur AmphB vs SB 2004 (20) had cure rates of 100% by both ITT and PP (60 patients, 1 mg AMB/kg daily for 20 days). The cure rates for eight trials and the nine arms of amphotericin B comparative trials are given in Figure 10. The cure rates of amphotericin B when compared to other drugs is depicted in Figure 13, and Figure 14 shows the Funnel plots of six-month ITT failure rates in trials comparing amphotericin B to other drugs with relative risk and 95% confidence Intervals.
Safety: Adverse events were diarrhoea (13 cases from two studies, 0.7%), vomiting (27 cases from two studies, 1.3%), elevated AST (84 cases from 3 studies, 4.1%), ALT (62 cases from three studies, 3%), creatinine (85 cases,4.1%) and BUN (43 cases, 2.1%), hepatotoxicty (two cases from two studies, 0.1%), nephrotoxicity (43 cases from two studies, 2.1%) and thrombocytopenia (one case, 0.05%). One case of death due to gastroenteritis and diarrhoea occurred in the study "Sundar AmphB vs Par2007" (0.05%). Rashes, anorexia, (eight cases each, 0.4%) fever and chills related to infusion (94 cases, 4.6%) and hypothermia (1 case, 0.05%) were also reported. (See Table 5.)
Liposomal amphotericin B
We identified six trials and 11 treatment arms for liposomal amphotericin B (AmBisome®). There were two comparative trials (two arms), three dose-finding (eight arms) and one non-comparative. A total of 476 patients were enrolled (8.3% of the database) and 474 patients were evaluable (8.8% of evaluable patients). (Tables 1 and 2; Figures 5 and 6.)
The dose-finding trial Sundar AmBi single vs daily 2001 had cure rates of 91.3% by both ITT and PP (46 patients) for group 1(5 mg/kg as single infusion). For group 2 (1 mg/kg for 5 days) the cure rates are 93.3% by both ITT and PP (45 patients). For Sundar AmBi, 3 regimens 2002 the cure rates are 89.3%, 92.9% and 96.4% by both ITT and PP for group A (0.75 mg/kg per day for 5 days (cumulative dose, 3.75 mg/kg) group B (1.5 mg/kg per day for five days (cumulative dose, 7.5 mg/kg) and group C (3.0 mg/kg per day for five days (cumulative dose, 15.0 mg/kg) respectively. (All three groups had 28 patients each.) In the case of Thakur AmBi,3 regimens 1996 group 1(2mg/kg on days 1 to 6, and 10 (total dose 14 mg/kg) and group 3 (2mg/kg on days 1, 5 and 10 (total dose 6 mg/kg) (10 patients each) had cure rates of 100% by both ITT and PP. Group 2 (2mg/kg on days 1,2,3,4and 10 (total dose 10 mg/kg) had a cure rate of 90% and 100% by ITT and PP respectively. For Sundar AmphB, Conv vs lipid 2004 (51 patients) (2 mg/kg/day for five days), the cure rates were 96.1% and 98% by ITT and PP respectively. Cure rates were 100% by both ITT and PP for Thakur AmBi vs AmphB 2001 (17 patients) (15 mg/kg, single dose). The trial Sundar AmBi non-comp 2003( 7.5mg/kg single infusion) had cure rates of 90.1% by both ITT and PP (203 patients). (Table 3.) Figure 15 depicts the efficacy of AmBisome.
Safety: The most common adverse event was infusion-related fever and chills (78 cases, 16.3%). Other adverse events included rigors (49 cases from two studies, 10.3%), vomiting (34 cases from 3 studies, 7.15%) and backache (10 cases from 2 studies, 2.1%). (See Table 5.)
Comparative trials: Amphotericin B deoxycholate was compared to other treatments in eight trials (nine comparisons: miltefosine=3; paromomycin=1; AmBisome=2; sodium stibogluconate=3) involving a total of 1675 patients (Figure 14) There was no significant difference with miltefosine on either aggregate data or individual comparisons and with AmBisome. Amphotericin B was better than paromomycin (only one study, RR(95%CI)=0.22(0.05-0.94)). However, the study was designed as a non-inferiority trial and paromomycin was within the pre-defined delta to declare it not inferior to amphotericin B. Amphotericin B was consistently more effective than sodium stibogluconate (aggregate RR(95%CI) 0.02(0.00-0.11). There was no significant heterogeneity (Table 4.) All comparisons display around the line of equality in the L'Abbé plot except the three studies against sodium stibogluconate (Figure 14.)
Discussion and conclusion
Our analysis shows amphotericin B deoxycholate is effective but impractical, as it requires 15 injections and 30 days in hospital and is associated with both infusion-related and delayed toxicities. AmBisome® is safer than plain amphotericin B and is very effective. Miltefosine is as effective as amphotericin B and is the only drug that has been tested in a Phase 4 study; in these conditions, effectiveness was lower than efficacy. Paromomycin is effective both alone and combined with sodium stibogluconate and was shown not to be different from amphotericin B using a non-inferiority trial design (the direct comparison used here may not be appropriate.) Sodium stibogluconate is clearly lost to parasite resistance in Bihar but recent data from other areas were not available. The only study from Bangladesh (27) was done in 1988-1990 but published in 1993.
Limitations
Limitations of the review
In review only three studies done outside India could be identified, all on sodium stibogluconate, none recent, and none on any of the three drugs (AmBisome®, miltefosine and paromomycin) that the review found were potentially beneficial for the elimination campaign. It is unlikely that any studies were missed. While the results of this systematic review are up to date, comprehensive and informative for the elimination campaign in India, it has little more to offer for Bangladesh and Nepal in terms of current status of sodium stibogluconate responsiveness of Leishmania isolates and in terms of efficacy and effectiveness of other leading drugs in those countries. A limitation with respect to Bangladesh and Nepal is the lack of studies for drugs other than sodium stibogluconate.
Limitations of the included studies
All studies meeting the inclusion criteria were included, regardless of quality. Extracting full information on the quality of studies and methods was not always easy. Not all studies gave sufficient information on patient attrition, numbers enrolled, and those that were evaluable (intent to treat versus per protocol analysis). Safety was also unevenly reported. This limitation does unfortunately reduce the strength of the evidence for the effectiveness of the treatments evaluated in this review.
Implications for public health, practice and further research
Rigorously conducted reviews of data on the effectiveness of health care interventions are a valuable tool to assist and inform policy, practice and research decisions. This is the first systematic review of clinical studies done in the Indian subcontinent that includes studies from Nepal and Bangladesh. This systematic review confirms that safe and efficacious treatment options are currently available in India and should be tested and made available in Nepal and Bangladesh. The findings of this review indicate that treatment policies should consider the use of AmBisome, miltefosine and paromomycin.
Miltefosine is the only oral drug and India was the first country to approve its use in 2002 (36). The Phase 4 clinical trial published in June 2007 supports its use in an outpatient setting where VL is endemic (24). Changing to an ambulatory setting, from the current inpatient treatment for VL patients in India, would allow reaching out to more patients who would otherwise receive no or inappropriate treatment – a major factor for the success of the elimination programme.
The oral bioavailability of miltefosine is both a blessing and a curse, as this facilitates coverage but can lead to misuse which can be deleterious to the drug's safety and therapeutic lifespan (42). Therefore, miltefosine should only be distributed under supervision by properly educated prescribers. Currently, a few days' supply of miltefosine can be bought from retail medical shops without a prescription (4,36). Patients not aware of the consequences of incomplete treatment, contraindications and adverse effects, will tend to buy a few days worth of medication and will discontinue treatment as soon as the symptoms are relieved (42), which will inevitably lead to resistance and toxicity (43).
There is a concern regarding use of miltefosine in women of child bearing age. In this subcontinent the correct status of pregnancy is not known to many women. Ensuring effective contraception during treatment and afterwards for a reasonable time period is mandatory. In current socioeconomic conditions women cannot always decide their time of conception. A long acting contraceptive such as IM injections should be practised routinely to avoid any accidental mishap when other forms of contraception are not possible (42).
The cost of a full miltefosine course is US$145 for an adult private patient (4,42). A special discount (US$64 for a full course treatment) was obtained through WHO for approximately 20,000 treatments (36). However, a definitive agreement on pricing has not been reached.
Paromomycin is an old aminoglycoside which compares well in terms of efficacy and safety to the other leading treatments. Its main advantage is the very competitive price (US$10 for an adult treatment). On the other hand, the main drawback is three weeks of daily injections (though costs, burden to health providers and inconvenience to patients can be reduced by treating on an outpatient basis) (4).
More emphasis should be placed on the potential role of AmBisome® and the necessity of a reduced or subsidized price. Even after the current reduction of price, it is still beyond the reach of the poor in the Indian subcontinent. It is the most effective and safe drug but needs to affordable. Liposomal amphotericin B is very effective at 10-15mg/kg given at multiple doses. The single dose is appealing for practical and cost reasons but it will leave around 10% of patients untreated and may trigger parasite resistance.
There are both theoretical foundations and clinical evidence in favour of the use of combination therapies to protect antileishmanial drugs, especially in areas of anthroponotic transmission, like the Indian subcontinent where resistance could spread quickly (44). Despite the high efficacies of miltefosine, paromomycin and liposomal amphotericin B, there is always the danger of resistance developing with time, particularly if the dose adopted is too low or adherence is sub-optimal. Therefore, short-course multidrug regimens should be developed to ensure compliance and prolong the useful lifespan of these drugs. Overall dose and duration of treatment can be reduced by combining two drugs, which will result in lower direct and indirect cost to the patient. If an oral drug is part of the combination, hospitalization may be limited to the initial few days, with the patient continuing treatment at home, and returning to the hospital for check ups and weekly supplies of medication, using a tuberculosis-like DOT (directly observed treatment) strategy. Evidence is available to support the combination of antileishmanial drugs. (49) High cure rates can be achieved with a shortened course, as indicated in the trial of paromomycin with a failing sodium stibogluconate and a more recent Phase 2 trial of the sequential treatment with AmBisome followed by 7-14 days of miltefosine which produced cure rates of 96% or greater (49).
Drugs are not the only control tool; other policy measures like active case finding and treatment, effective vector control, patient education are paramount to the success of the vsceral leishmaniasis elimination programme.
There is a clear need to document efficacy and safety of treatment options outside India. Only two studies, both on sodium stibogluconate, were done in Nepal and none in Bangladesh during 1990-2006 (the study from Bangladesh was published in 1993 but done earlier). There is a lack of information on whether the efficacy of sodium stibogluconate has decreased in Bangladesh and Nepal as it did in Bihar, and no information on miltefosine (which is the recommended treatment choice) and other drugs like AmBisome and paromomycin.
Once drugs are distributed, monitoring their use, compliance, safety and tolerability through pharmacoepidemiology and pharmacovigilance is essential. The safety profile in practice may be different from the controlled conditions of clinical trials, where difficult patients are excluded and adherence and practices optimized. In addition, rare events will only be seen after large numbers of patients are exposed. We need more data on the effectiveness of drugs when used in a real life setting.
Summary boxes
What has been learned from this review?
- Approximately 60% of the annual global burden of VL occurs in the Indian subcontinent.
- Current treatment modalities include drugs injected intravenously (amphotericin B deoxycholate or in lipid formulations) or intramuscularly (paromomycin, and sodium stibogluconate) and an oral drug (miltefosine).
- Liposomal amphotericin B (AmBisome®) is safer than basic amphotericin B and is effective but is also very expensive.
- Miltefosine is as effective as amphotericin B and is the only oral drug and the only drug that has been tested in a Phase 4 study; in these conditions, effectiveness may be lower than efficacy in trials, when drug intake is supervised.
- Paromomycin is effective both alone and combined with sodium and is very cheap but must be given by injection; it has been shown not to be different from amphotericin B using a non-inferiority trial design.
Implications for public health practice
- This systematic review confirms that safe and efficacious treatment options are currently available in India and these should be tested and made available in Nepal and Bangladesh.
- Treatment policies should consider the use of AmBisome, miltefosine and paromomycin. Sodium stibogluconate is lost to resistance in Bihar, but there is no recent information from outside India.
- Miltefosine should only be distributed under the supervision of educated prescribers to avoid misuse and in order to maximize its therapeutic lifespan (limit the risk of resistance and serious toxicities.)
- Prices of drugs need to reduced or subsidized by the government so as to reach as many patients as possible.
Priority research areas
- Clinical research is needed to identify suitable treatment options in Nepal and Bangladesh, as well to determine resistance to sodium stibogluconate.
- Drug combinations need to be tested in order to protect drugs against resistance and prolong their lifespan of effective use.
- Research on the effectiveness of drugs when used in a real life setting, should be conducted, as conditions in practice are different from the controlled conditions of clinical trials.
- Strong, active and continuous pharmacovigilance is needed when new drugs are distributed to document safety and rational use.
- The methodological quality and consistency of clinical trials is paramount.
- More emphasis should be given to the systematic collection of clinical and laboratory safety information.
References
1. World Health Organization (2002). World Health Report 2002; Reducing Risks, Promoting Healthy Life. WHO, Geneva, Switzerland. pp186-192. [ Links ]
2. Sundar S, Mondal D, Rijal S, Bhattacharya S, Ghalib H, Kroeger A, Boelaert M, Desjeux P, Richter-Airijoki H, Harms G (2008). Implementation research to support the initiative on the elimination of kala azar from Bangladesh, India and Nepal; the challenges for diagnosis and treatment. Trop Med Int Health;13(1):2-5. [ Links ]
3. Business plan: Business line 10: Visceral leishmaniasis elimination Draft Business Plan for JCB , May, 2007,WHO/TDR. http://apps.who.int/tdr/documents/bl-2007-annual-reports/BL10-annual-report-2007.pdf. Accessed online, 16 June, 2008. [ Links ]
4. Olliaro PL, Guerin PJ, Gerstl S, Haaskjold AA, Rottingen JA, Sundar S (2005). Treatment options for visceral leishmaniasis: a systematic review of clinical studies done in India, 1980-2004. Lancet Infect Dis;5(12):763-774. [ Links ]
5. Singh SP, Reddy DC, Rai M, Sundar S (2006). Serious underreporting of visceral leishmaniasis through passive case reporting in Bihar, India. Trop Med Int Health;11:899-905. [ Links ]
6. Alvar J, Yactao S , Bern C (2006). Leishmaniasis and poverty. Trends Parasitol;22:552–557. [ Links ]
7. WHO/TDR. Press release: Elimination of kala-azar from endemic countries in the south-east Asia region. Health ministers' sign memorandum of understanding. Geneva/New Delhi, May 18, 2005. http://www.who.int/tdrold/diseases/leish/press_release.htm. Accessed online June 10, 2008. [ Links ]
8. World Health Organization, South East Asia Regional Office (2006). Kala Azar: Why Kala Azar Elimination is Possible in South Asia Countries? http://www.searo.who.int/en/Section10/Section2163_11671.htm. Accessed online 10 June, 2008. [ Links ]
9. Davidson RN (1998). Practical guide for the treatment of leishmaniasis. Drugs; 56:1009-1018. [ Links ]
10. Murray HW (2000). Treatment of visceral leishmaniasis (kala-azar): a decade of progress and future approaches. Int J Infect Dis;4:158-177. [ Links ]
11. Guerin PJ, Olliaro P, Sundar S, et al (2002). Visceral leishmaniasis: current status of control, diagnosis, and treatment, and a proposed research and development agenda. Lancet Infect Dis 2002;2:494-501. [ Links ]
12. Jha TK, Olliaro P, Thakur CP, Kanyok TP, Singhania BL,Singh IJ, Singh NKP, Akhoury S, Jha S (1998). Randomised controlled trial of aminosidine (paromomycin) v sodium stibogluconate for treating visceral leishmaniasis in North Bihar, India. BMJ;316(7139):1200-1205. [ Links ]
13. Mishra M, Biswas UK, Jha AM, Khan AB (1994). Amphotericin versus sodium stibogluconate in first-line treatment of Indian kala-zar: Lancet;344(8937):1599-1600. [ Links ]
14. Singh UK, Prasad R, Mishra OP, Jayswal BP (2006). Miltefosine in children with visceral leishmaniasis: a prospective, multicentric, cross-sectional study. Indian J Pediatr;73(12):1077-1080. [ Links ]
15. Sundar S, Jha TK, Thakur CP, Sinha PK, Bhattacharya SK (2007). Injectable paromomycin for Visceral leishmaniasis in India : N Engl J Med;356(25):2571-2581. [ Links ]
16. Sundar S, Mehta H, Suresh AV, Singh SP, Rai M, Murray HW (2004). Amphotericin B treatment for Indian visceral leishmaniasis: conventional versus lipid formulations: Clin Infect Dis;1:38(3):377-383. [ Links ]
17. Thakur CP (2001). A single high dose treatment of kala-azar with Ambisome (amphotericin B lipid complex): a pilot study: Int J Antimicrob Agents;17(1):67-70. [ Links ]
18. Sundar S, Jha TK, Thakur CP, Engel J, Sindermann H, Fischer C, Junge K, Bryceson A, Berman J (2002). Oral miltefosine for Indian visceral leishmaniasis. N Engl J Med;347(22):1739-1746. [ Links ]
19. ThakurCP,Sinha GP,Sharma V,Pandey AK, Kumar M, Verma BB (2002). Evaluation of amphotericin B as a first line drug in comparison to sodium stibogluconate in the treatment of fresh cases of kala-azar. Ind J Med Res;97:170-175. [ Links ]
20. Thakur CP, Narayan S (2004). A comparative evaluation of amphotericin B and sodium antimony gluconate, as first-line drugs in the treatment of Indian visceral leishmaniasis .Ann Trop Med Parasitol;98(2):129-138. [ Links ]
21. Thakur CP, Kanyok TP, Pandey AK, Sinha GP, Messick C, Olliaro P (2000). Treatment of visceral leishmaniasis with injectable paromomycin (aminosidine). An open label randomized phase II clinical study. Trans R Soc Trop Med;94,432-433. [ Links ]
22. Thakur CP, Kanyok TP, Pandey AK, Sinha GP, Zaniewski AE, Houlihan HH, Olliaro P (2000). A prospective randomized, comparative, open-label trial of the safety and efficacy of paromomycin (aminosidine) plus sodium stibogluconate versus sodium stibogluconate alone for the treatment of visceral leishmaniasis. Trans R Soc Trop Med Hyg;94:429-431. [ Links ]
23. Bhattacharya SK, Jha TK,Sundar S,Thakur CP,Engel J, Sindermann H,Junge K,Karbwang J, AnthonyD M, Bryceson A, Berman J D (2004). Efficacy and Tolerability of Miltefosine for Childhood Visceral Leishmaniasis in India. Clin Infect Dis;38:217-221. [ Links ]
24. Bhattacharya SK, Sinha PK, Sundar S, Thakur CP, Jha TK, Pandey K, Das VR, Kumar N, Lal C, Verma N, Singh VP, Ranjan A, Verma RB, Anders G, Sindermann H, Ganguly NK (2007). Phase 4 trial of miltefosine for the treatment of Indian visceral leishmaniasis.J Infect Dis;196(4):591-598. [ Links ]
25. Rijal S, Chappuis F, Singh R, Bovier PA, Acharya P, Karki BM, Das ML, Desjeux P, Loutan L, Koirala S (2003). Treatment of visceral leishmaniasis in south-eastern Nepal: decreasing efficacy of sodium stibogluconate and need for a policy to limit further decline. Trans R Soc Trop Med Hyg;97(3):350-354. [ Links ]
26. SundarS,Jha TK,ThakurCP,Mishra M,Singh VP, Buffels R (2003). Single-dose liposomal amphotericin B in the treatment of visceral leishmaniasis in India: a multicenter study. Clin Infect Dis;37(6):800-804. [ Links ]
27. Chowdhury M, A J, Alam M N Hussain A, Uddin A K M Rahman (1993). A study on the treatment of Bangladeshi Kala-azar patients with different dosage regiments of sodium antimony gluconate: Bangladesh J of Medicine;4(1):1-5. [ Links ]
28. Jha TK, Sundar S,Thakur CP,Bachmann P,Karbwang J,Fischer C,Voss A, Berman J (1999). Miltefosine, an oral agent, for the treatment of Indian visceral leishmaniasis: N Engl J Med;341(24):1795-1800. [ Links ]
29. Karki P,.Koirala S,Parija SC, Hansdak SG and DasML (1998). A thirty day course of Sodium Stibogluconate for Treatment of Kala Azar in Nepal. South East Asian J Trop Med Pub Health;29(1):154-158. [ Links ]
30. Sundar S, Agrawal G,Rai M,Makharia MK, Murray HW (2001). Treatment of Indian visceral leishmaniasis with single or daily infusions of low dose liposomal amphotericin B: randomised trial. BMJ;323:419-422. [ Links ]
31. Sundar S, Jha TK, Thakur CP, Mishra M, Singh VR, Buffels R (2002). Low-dose liposomal amphotericin B in refractory Indian visceral leishmaniasis: a multicenter study : Am J Trop Med Hyg;66(2):143-146. [ Links ]
32. Sundar S, Chakravarty J, Rai VK, Agrawal N, Singh SP, Chauhan V, Murray HW (2007). Amphotericin B treatment for Indian visceral leishmaniasis: response to 15 daily versus alternate-day infusions: Clin Infect Dis;45(5):556-561. [ Links ]
33. Sundar S, Jha TK, Sindermann H, Junge K, Bachmann P, Berman J (2003). Oral miltefosine treatment in children with mild to moderate Indian visceral leishmaniasis: Pediatr Infect Dis J;22(5):434-438. [ Links ]
34. Thakur CP, Pandey AK, Sinha GP, Roy S, Behbani K, Olliaro P (1996). Comparison of three treatment regimens with liposomal amphotericin B (AmBisome) for visceral leishmaniasis in India: a randomized dose-finding study: Trans R Soc Trop Med Hyg;90:319-322. [ Links ]
35. E-DRUG (2007). Price reductions for drugs for leishmaniasis. http://www.essentialdrugs.org/edrug/archive/200705/msg00062.php. Accessed online, 2 July, 2008. [ Links ]
36. Sundar S, Olliaro PL (2007). Miltefosine in the treatment of leishmaniasis: Clinical evidence for informed clinical risk management. Ther Clin Risk Manag;3(5):733-740. [ Links ]
37. Institute for One World Health (2007). Research on New Treatment for Neglected Disease Published in The New England Journal of Medicine (Press Release, 21 June, 2007.) http://www.oneworldhealth.org/press_releases/release/pr_1226357893. Accessed online, 2 July, 2008. [ Links ]
38. Interview with Mari Carmen Viñoles, MSF General Coordinator Bihar, India. "New kala azar project in India: The disease of the "untouchables". http://www.msf.org.uk/New_kala_azar_project_in_India_the_disease_of_the_untouchables.news. Accessed online, July 2, 2008. [ Links ]
39. Sundar S, Sinha PR, Agrawal NK, et al. (1998). A cluster of cases of severe cardiotoxicity among kala-azar patients treated with a high-osmolarity lot of sodium antimony gluconate. Am J Trop Med Hyg 59:139–143. [ Links ]
40. Rijal S, Chappuis F, Singh R, et al. (2003). Sodium stibogluconate cardiotoxicity and safety of generics. Trans R Soc Trop Med Hyg;97:597-598. [ Links ]
41. Sundar S, Thakur BB, Tandon AK, et al. (1994). Clinicoepidemiological study of drug resistance in Indian kala-azar. BMJ; 308(6924):307. [ Links ]
42. Sundar S, Murray HW (2005). Availability of miltefosine for the treatment of kala-azar in India. Bull World Health Organ;83:394-395. [ Links ]
43. Seifert K, Matu S, Javier Perez-Victoria F et al (2003). Characterisation of Leishmania donovani promastigotes resistant to hexadecylphosphocholine (Miltefosine). Int J Antimicrob Agents;22:380-387. [ Links ]
44.Bryceson A (2001). A policy for leishmaniasis with respect to the prevention and control of drug resistance. Trop Med Int Health;6:928-934. [ Links ]
45. Alvar J, Croft S, Olliaro P (2006). Chemotherapy in the treatment and control of leishmaniasis. Adv Parasitol;61:223-274. [ Links ]
46. World Health Organization, South East Asia Regional Office (2007). Trends of Kala Azar in India. http:/www.searo.who.int/LinkFiles/Kala_azar_Trends_India.pdf. Accessed online 2 July, 2008. [ Links ]
47. Trends of Kala Azar in Bangladesh http://www.searo.who.int/LinkFiles/Kala_azar_Trends_Bangladesh.pdf [ Links ]
48. World Health Organization, South East Asia Regional Office (2007). Trends of Kala Azar in Nepal http://www.searo.who.int/LinkFiles/Kala_azar_Trends_Nepal.pdf. Accessed online 2 July, 2008. [ Links ]
49. Sundar S, Rai M, Chakravarty J, Agarwal D, Agrawal N, Vaillant M, Olliaro P, Murray HW (2008). New Treatment Approach in Indian Visceral Leishmaniasis: Single-Dose Liposomal Amphotericin B Followed by Short-Course Oral Miltefosine. Clin Infect Dis 47(8):1000-1006. [ Links ]
50. Sundar S, Chatterjee M (2006). Visceral leishmaniasis-current therapeutic modalities. Indian J Med Res;123:345-352. [ Links ]
Corresponding author: Messiah M Cheeran, cmessiah@gmail.com.